- Home
- Patient Care
- Services
- Sports Medicine
- Overview
- Knee
- Articular Cartilage Restoration
Articular Cartilage Restoration
 Download PDF
Download PDF
Overview
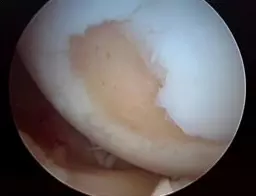 Articular cartilage is the smooth, white tissue that covers the ends of bones where they come together to form joints. Healthy cartilage in our joints makes it easier to move, allowing the bones to glide over each other with very little friction. Articular cartilage can be damaged by injury or normal wear and tear. Because cartilage does not heal itself well, surgical techniques have been developed to stimulate the growth of new cartilage. The image to the right shows a defected cartilage.
Articular cartilage is the smooth, white tissue that covers the ends of bones where they come together to form joints. Healthy cartilage in our joints makes it easier to move, allowing the bones to glide over each other with very little friction. Articular cartilage can be damaged by injury or normal wear and tear. Because cartilage does not heal itself well, surgical techniques have been developed to stimulate the growth of new cartilage. The image to the right shows a defected cartilage.
Patient eligibility
Most candidates for articular cartilage restoration are young adults with a single injury, or lesion. Older patients, or those with many lesions in one joint, are less likely to benefit from the surgery.
Treatment Options
We are the only orthopedic sports medicine team in the region that specializes in articular cartilage restoration. Our sports medicine specialists are fellowship-trained and have experience in performing the most complex procedures. We are leaders in providing the most advanced sports medicine treatments as a result of our continuous orthopedic research.
 Arthroscopy versus open incision
Arthroscopy versus open incision
Many procedures to restore articular cartilage are done arthroscopically. During arthroscopy, three small puncture incisions are made around the joint using an arthroscope. A fiberoptic camera is inserted into the joint to visualize all structures and restore the cartilage. Some procedures require the surgeon to have more direct access to the affected area, requiring longer, open incisions. Sometimes it is necessary to address other problems in the joint, such as meniscal or ligament tears, while cartilage surgery is being done. We discuss options with patients to determine what kind of procedure is right for them.
Common Procedures for Articular Cartilage Restoration
Microfracture
Goal: Stimulate the creation of a blood clot into the cartilage defect. The cells in the clot have the potential to mature into new cartilage cells that ultimately fill the defect.
Candidates: Patients ages 40 years and under with an acute, isolated cartilage defect without surrounding arthritis.
Technique: Holes are made in the subchondral bone beneath the cartilage. This action creates a healing response. New blood supply can reach the joint surface, bringing with it new cells that will form the new cartilage.
Abrasion Arthroplasty
Goal: Stimulate the creation of a blood clot that contains cells with the potential to form new cartilage within the defect.
Candidates: Candidates for abrasion arthroplasty are similar to that of microfracture.
Technique: High speed burrs are used to remove the damaged cartilage and reach the subchondral bone in order to stimulate blood cells that create a healing response. Abrasion arthroplasty can be done through arthroscopic visualization.
Autologous Chondrocyte Implantation (ACI)
Goal: Regenerate cartilage using the patient’s own cells.
Candidates: Most useful for younger patients who have single defects larger than two centimeters in diameter.
Technique: ACI is a two-step procedure in which the patient’s normal cartilage cells are harvested, grown and expanded in a laboratory, and then re-implanted into the cartilage defect. The advantage of using the patient’s own cells is that there is no danger of a patient rejecting the tissue. It does have the disadvantage of being a two-stage procedure that requires an open incision for implantation. It also takes several weeks to complete.
Osteochondral Autograft Transplantation
Goal: Healthy cartilage is transferred from one part of the joint to another.
Candidates: Individuals with smaller cartilage defects.
Technique: A healthy bone and cartilage plug, or graft, is taken from an area of the bone that is non-weightbearing. The graft is taken as a cylindrical plug of cartilage and subchondral bone (osteochondral autograft). It is then matched to the surface area of the defect and impacted into place. This leaves a smooth cartilage surface in the joint. A single plug of cartilage may be taken or a procedure using multiple plugs, called ‘mosaicplasty’, may be performed.
Osteochondral Allograft Transplantation
Goal: Healthy cartilage is transferred from a donor into the joint.
Candidates: Individuals with a large cartilage defect greater than two centimeters in diameter.
Technique: A larger tissue graft comprised of intact bone and cartilage is taken from a cadaver donor. In the laboratory it is sterilized and prepared, and tested for any possible disease transmission. It can be shaped into a cylindrical graft that fits the exact contour of the defect and then press fit into place. Allografts are typically done through an open incision.
New Techniques for Cartilage Restoration
Goal: Healthy pieces of minced or freeze-dried cartilage are transferred from a donor into the joint.
Candidates: individuals with a large cartilage defect greater than 2 centimeters in diameter.
Technique: Pieces of minced cartilage or freeze-dried cartilage paste is taken from a cadaver donor. In the laboratory the cartilage specimen is finely minced or ground into a fine powder that is mixed with the patient’s plasma to form a cartilage paste. The grafts are then shaped to fit the exact contour of the defect and ‘glued’ into place with a biologic glue. This is typically performed through an open incision.
Recovery and outlook
After surgery, the joint surface must be protected while the cartilage heals. If the procedure was done on the knee or ankle, the patient may not be able to put weight on the affected leg. Crutches can be used to move around for the first two or three months after surgery. After surgery, we provide physical therapy to help restore mobility and strength to the affected joint.
During the first weeks after surgery, patients may begin continuous passive motion therapy. A continuous passive motion machine constantly moves the joint through a controlled range of motion. As healing progresses, therapy focuses on strengthening the joint and the muscles that support it. It may be several months before a patient can safely return to sports activity.