- Home
- Patient Care
- Services
- Pediatric and Adolescent Orthopedic Surgery
- Overview
- Knee Education Overview
- ACL
ACL Reconstruction
OFFICE NUMBERS:
Debbie Krenning, Medical Assistant (314)454-4191
Kim Cordia, Nurse Educator (314)454-5221
Inpatient
Amy Hanson, Nurse Coordinator (314)454-4408
Saint Louis Children’s Hospital
Appointment Desk (314)454-2500
Main Number (314)454-6000
Same Day Surgery (314)454-6174
10th Floor (314)454-6038
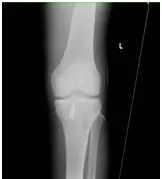
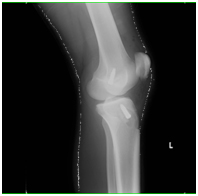
What is the Anterior Cruciate Ligament?
The ACL is ligament that, along with other structures, helps maintain a stable joint during the knee’s range of motion. The other main knee ligaments are: posterior cruciate ligament, medial collateral ligament and the lateral collateral ligament.
Where is the anterior cruciate ligament?
The ACL is completely within the knee joint and starts at the lateral femoral condyle of the femur (thigh bone) and attaches to the tibia (shin bone). The blood supply to the ACL is through its bony attachments and hence does not heal well.
What is the function of the ACL?
Due to the attachments its primary responsibility is to limit forward movement of the tibia on the femur. In addition the ACL provides rotational stability to the knee during cutting activities.
How common are the ACL injuries?
The incidence is 0.3-0.38 per 1000 individuals per year. Bony injuries of the ACL occur in 3 out of 100,000 children per year. Published studies document that skeletally immature patients account for 3-4% of all ACL tears.
What sports are associated with ACL injuries?
Football, soccer, skiing and basketball.
How does failure of the ACL occur in children?
Bony avulsion of the attachments of the ACL can occur in preadolescent children. Tears in the middle of the ligament are more common in adolescents. The mechanism of injury is generally hyperextension, sudden deceleration, or an angular-rotational force to the knee.
What is the natural history of the ACL deficient knee in a skeletally immature patient?
Not well defined due to the small number of injuries. For adolescents it seems to be similar that in young adults. Episodes of “giving way” are reported to be 33-86% of patients with ACL tears treated non-operatively. Activity level, not age, is the primary risk factor for recurrent instability. Because adolescents are very active, conservative treatment will fail in a great number of patients. A relatively inactive adolescent, however, may have a very satisfactory outcome with ligament reconstruction.
Should an ACL sprain be treated by casting the knee?
The ACL has very limited capacity to heal. The blood supply comes from each end and is often disrupted with the sprain because it is located in the center of the knee joint. Cast immobilization has not been show to improve outcome. Following acute injury, the knee should be rested with a brace or immobilizer until swelling and pain subsides.
What are the management options for an isolated tear in the middle of the ACL in a skeletally immature child?
In absence of a torn meniscus, ACL injuries are best managed with activity modification and observation. Repair of intrasubstance ligament tears is at best controversial and will have a high rate of failure. Failure of nonoperative management (pain, instability, meniscal tears, etc…) should undergo surgical stabilization. In the skeletally immature individuals, tunnels cross the growth plates and are therefore at risk for growth plate injury which could result in shortening or angular deformity. The reconstruction graft should not place a bone block across the growth plate which would promote growth plate bar. The use of hamstring tendons are the preferred graft in skeletally immature individuals.
What if there is a meniscal tear with the ACL injury?
Current standard of care is to repair the meniscus and reconstruct the ACL. Isolated meniscal repairs without ACL reconstructions are occasionally performed however there is an increased risk of the meniscus not healing or re tearing when the individual resumes athletic activities.
What are the issues with ACL reconstructions?
Anatomic reconstruction of the ligament best restores knee stability and motion. Anatomic reconstruction means tibial and femoral bone tunnels.
Can and ACL injury be prevented?
Sports which involve cutting and deceleration maneuvers place significant stress onto the ACL ligament. No published studies to date have shown prophylactic bracing can prevent ACL injuries. The only known method is to limit potential injury to the ACL is to minimize participation in at-risk sports, such as soccer, football, skiing and basketball.
Can ACL reconstruction tears, like the native ACL?
Yes the ACL reconstruction ideally is placed into the exact same location as the original ACL. Forces which caused the ACL tear can also cause damage to the ACL reconstruction. Re-injury rates however have been documented very low.
Will ACL reconstructions prevent arthritis of the knee joint if it is performed?
No long-term studies have been performed to document this effect. Theoretically by reconstruction the ACL the knees motion and stability is restored, thereby minimizing abnormal motion and instability. By eliminating instability, the ACL reconstruction may delay the onset of knee joint arthritis
ACL Reconstruction Surgery
What type of anesthesia?
General Anesthesia which means that you will fall asleep and the anesthesiologist will wake you up when the surgery is complete. You will not wake up until the procedure is complete.
How will my pain be managed?
· Femoral Nerve Block is added to minimize postoperative pain. This nerve block will have sustained effects for up to 16 hours. When the nerve block begins to wear off one will feel a “tingly”or “funny bone” sensation.
· It is at this point that either intravenous or oral pain medication should be taken.
Will I get sick after surgery?
Nausea and vomiting occurs in approximately 1/3 of patients. Medications will be available to minimize any nausea and vomiting.
When can I eat after surgery?
When you awake from anesthesia… remember the possibility of nausea and vomiting after surgery so go very slow with eating and drinking. It is best to choose bland foods that are easier on the stomach.
Will I get pain medications to go home with after surgery?
Yes the narcotic prescription will be supplied that should be adequate enough until your first follow up appointment.
What if the pain prescription is not enough?
1) Limb must be elevated above the level of heart (with pillows) and ice on the knees
2) You may also take ibuprofen/Nuprin/motrin to supplement the narcotic prescription. Follow the directions on the ibuprofen bottle independently of the narcotic.
3) If the narcotic and ibuprofen is not enough to control the pain contact either Debbie, Kim or the on call physician for recommendations.
What should I do if I am nauseated and vomiting at home?
Go slow with the eating and drinking. The narcotics prescribed for pain frequently cause nausea and vomiting. If you are taking any ibuprofen stop taking it. If this persists and is not improving despite slowing the by mouth intake, call Debbie, Kim or the on call physician.
How do I get around after surgery?
Crutches…You may put the operated leg onto floor for balance. Full weight bearing is allowed but is usually not possible for at least 1-2 weeks due to pain.
Should I change the dressings or brace at home?
No leave the brace and postoperative dressings intact until your first followup visit. These will be changed at the first post operative visit which is usually between 3 and 5 days.
How do I take a bath or shower?
Until the first post operative appointment sponge baths are recommended in order to keep the brace and dressings dry.
Are there any things I should watch for when I go home?
· numbness tingling …elevate leg and if it persists you may loosen ace wrap and brace
· coloration of toes …should be pink and warm
· fever
· rash
· drainage from wound
When Can I go back to school?
Most patients who undergo an ACL reconstruction return to school between 6-8 days. If it is during the school year, contact the school to see what accommodations they can provide (such as additional set of books, elevator key, help to and from class