Vertebral Body Stapling
What is Vertebral Body 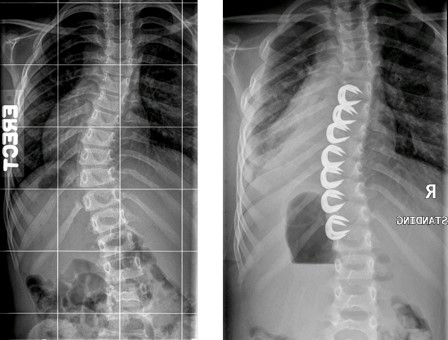 Stapling?
Stapling?
- A new, non-fusion technique used for the management of scoliosis in the thoracic and lumbar spine in skeletally immature patients.
- The concept of stapling the anterior vertebral growth plates for growth modulation and curve stabilization has proven to be effective in animals and humans on the convex side of the scoliosis.
- The effect of the staple is to reduce the rate of growth.
This is a possible alternative to bracing for patients who are at risk for a speedy progression of the curve, and who may need a spinal fusion in the future.
This procedure allows for preserved motion and less chance of back pain in adulthood.
Who is a candidate?
- Idiopathic scoliosis
- A child older than 8 years
- A child who will still have years of growth:
- Boys up to 16 years
- Girls up to 14 years
- Curve less than 45 degrees
- Spine flexibility
- Neurologically normal individuals
Which curves can be stapled?
Both thoracic and lumbar curves.
Who designed the staple?
Dr. Randy Betz has worked to develop the current staple design. At present he and his associates have treated several hundred young scoliosis patients with this technique.
How effective is vertebral body stapling?
Based on personal discussions with Dr. Randy Betz, and his two publications on Vertebral Body Stapling in peer-reviewed journals, vertebral body stapling is equally effective as bracing.
What are the advantages of Vertebral Body Stapling?
Patients who undergo Vertebral Body Stapling do not need a brace and have an equal chance the scoliosis will not progress to need a spine fusion.
What are the disadvantages of Vertebral Body Stapling?
It is a surgery with all the inherent risks of surgery.
What type of metal are the staples?
They are a combination of nickel and titanium called NITINOL, for Nickel Titanium Naval Ordinance lab. Nitinol has unique thermodynamic properties that allow it to change it shape based on the temperature or the metal. Near 0 degrees (in an ice bath) the tines of the staple are straight, and as the staples warm to body temperature the tines curve inward, and remain so in the body, in a C-shape.
What does the procedure involve?
- Patients will have a preoperative visit two to four weeks prior to procedure.
- The procedure is done under general anesthesia in the operating room.
- The procedure is performed with a thorascope
- A camera on the end of a long tube which enables surgery to be performed with a small incision on the chest.
- Staples are places over the convex side of the curve (usually the right side)
- The procedure is approximately two hours in length.
- A chest tube is placed to drain in air and fluid out of the chest for the first two days after surgery
- Patients will typically be in hospital for four days.
- Patients may spend the first night in the pediatric ICU.
- Patients will then go to the 10th floor (the orthopedic floor).
What happens to the staples?
In the largest series of patients at Shiners Hospital in Philadelphia ,no staples have broken or migrated. Due to the c-shape of the staples after they are implanted they cannot back out, loosen and travel in abdomen or chest.
What happens if the curves progress despite the stapling?
It depends on the amount of progression. Slight progression may occur, but likely will not need to be treated (such as a spine fusion). However, significant progression of the curves can still be treated with a spine fusion without difficulty.