Shilla Procedure
What is the Shilla Procedure?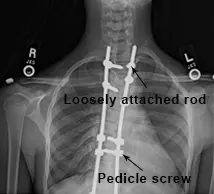
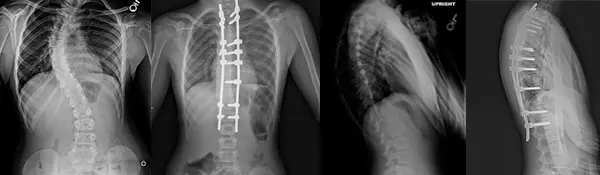
The Shilla procedure is a surgical procedure to treat scoliosis. The procedure uses rods and screws similar to a track and trolley system, which allows the spine to grow naturally while correcting a spinal curve. During the procedure, rods are attached to specific points in the spine with pedicle screws.
How long does the Shilla procedure take?
The Shilla procedure takes approximately four to six hours. Patients are typically kept at the hospital for five to seven days following the procedure.
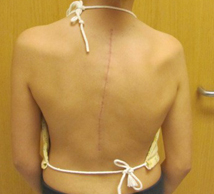
What does this incision look like?
The Shilla procedure involves a single incision in the back of the spine. After surgery, the patient’s incision is closed with dissolvable sutures and medical glue. The glue usually dissolves in 10 to 14 days. Before going home, the patient’s incision will be covered by a dressing.
Post-Operative Care
What is the typical post-operative care?
During their hospital stay, patients work with the hospital’s physical therapy team to monitor and improve movement/function. Once discharged, patients should take it easy and rest for four to six weeks following the surgery.
Will the patient be on pain medication post-operatively?
Yes. Children are followed by the pain service team while in the hospital. At first, the patient will be given medications through their IV. These will be discontinued after 24 hours and switched to oral medications.
The oral medications will be the same medications that the child is sent home on. Typically, most families report that their children continue to take their prescribed pain medication for 10-14 days while at home. However, this is variable and depends on each child’s pain tolerance.
Will the patient have spinal cord monitoring?
This is decided on a case-by-case basis. If the patient has normal neurological functioning prior to the procedure, then there will be spinal cord monitoring.
Broken Rods
Rod breakage is not uncommon. If a rod breaks, the patient might notice pain or discomfort. There could also be visible clinical changes.
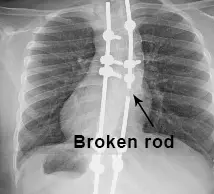
If a rod breaks, contact our office immediately so the patient may be seen in the office. The patient is evaluated at that time for the amount of spinal growth remaining, curve size and physical appearance of the spine, chest and trunk.
If a rod breaks, there are several treatment options available:
- The system can be removed.
- The system is removed and the patient has another Shilla placed.
- The system is removed and the patient goes on to a spinal fusion procedure.
Recovery and Outlook
How long are patients out of school?
Following surgery, patients are typically out of school approximately 10-14 days. Children should not return to school if they are still taking pain medications.