- Home
- Patient Care
- Services
- Hip & Knee
- Adult Reconstruction and Hip Preservation Overview
- Hip Dysplasia
Hip Dysplasia (Developmental Dysplasia of the Hip-DDH, Congential Dysplasia of the Hip-CDH)
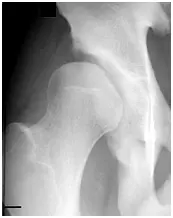
The normal hip (see figure) is a ball and socket joint with the femoral head (ball) well-seated and stable within the acetabulum (socket). Hip dysplasia includes a group of disorders that have deformities of the joint. Most commonly, hip dysplasia is characterized by a “shallow” socket (see figure) that does not adequately cover the femoral head. When the femoral head is not completely covered by the acetabulum, the hip is unstable, may become painful and eventually develop osteoarthritis.
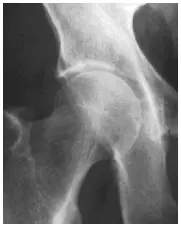
Normal hip with a well-covered,
stable femoral head. |
Dysplastic hip with a shallow socket and
unstable femoral head |
Normal Hip Joint
The bony structures of the hip joint (acetabular and femoral head) are covered with a smooth but durable covering called articular cartilage. Articular cartilage cushions the joint and allows the bones to move easily against each other. Around the rim of the hip socket is a ring of cartilage called the acetabular labrum. The acetabular labrum provides stability, maintains fluid pressure in the joint, and helps distribute weight to the femoral head. The entire hip joint is enclosed in strong tissue called the hip capsule. The inner surface of the hip capsule is lined with a smooth tissue called synovial membrane. The synovial membrane produces a lubricating fluid for smooth movement of the joint. Around the joint are ligaments that secure the femoral head in the hip socket.
Symptoms of Hip Dysplasia
Because of inadequate coverage of the femoral head, the weight supported by the hip is distributed over a smaller surface, creating an excessive load along the rim of the hip socket. Over time, this added load can cause joint cartilage to degenerate (break down), resulting in arthritis. Some common symptoms of hip dysplasia include:
-Pain in the groin or side of the hip
-A sensation of “catching” or “popping” with activity
-Worsening pain with sitting, walking or running
-Limping
-Increased difficulty with strenuous activities
Diagnosis of Hip Dysplasia
The diagnosis of symptomatic hip dysplasia is made by a complete medical history, a physical examination, and an X-ray evaluation. Sometimes other types of imaging, such as a magnetic resonance arthrogram (MRA) or a computed tomography (CT) scan may be required to make an accurate diagnosis.
Hip dysplasia may occur in people of all ages. Some people with symptoms of hip dysplasia may have been treated for hip problems as an infant or child. However, if there is some remaining deformity, symptoms may recur in adulthood and require treatment.
Treatment of Hip Dysplasia
Once a diagnosis of hip dysplasia is made, Dr. Clohisy can recommend the appropriate course of treatment. Hip dysplasia is often corrected by surgery. If hip dysplasia goes untreated, arthritis is likely to develop. Symptomatic hip dysplasia is likely to continue to cause symptoms until the deformity is surgically corrected.
Many patients benefit from a procedure called periacetabular osteotomy or PAO. The medical term “periacetabular” means “around the acetabulum” or “around the hip socket.” The term “osteotomy” refers to any procedure in which bone is cut. Thus, a PAO is a procedure where bone is cut around the hip socket.
What to Do If You Have Hip Dysplasia
Although hip dysplasia is one condition, every patient is unique, and hip dysplasia can become evident at different disease stages. If you are diagnosed with hip dysplasia, Dr. Clohisy will explain the specific problem with your hip and he will review the available treatment options. In general, if hip dysplasia is diagnosed early (prior to osteoarthritis), “joint preservation surgery” is considered. For example, a shallow hip socket can be surgically corrected with the PAO (see figure).
X-ray of 18-year-old male patient with acetabular dysplasia (shallow socket) of both hips. This patient had hip pain and limitation of sport activities.
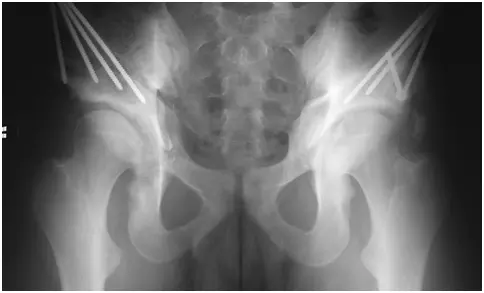
X-ray of both hips in the same patient after correction of the shallow sockets with PAO surgery. Note the improved coverage of the femoral head. This patient is now over five years from surgery and has an excellent clinical result for both hips.
If hip dysplasia is diagnosed later in the disease process and osteoarthritis (degeneration of the joint) is established, joint preservation surgery may not be an option. In this situation total hip replacement can be considered.
It is important to realize that hip dysplasia is usually a progressive condition that worsens with time. As the disease progresses, hip pain and activity limitations worsen. For this reason, early diagnosis and consideration of different treatment options is important.